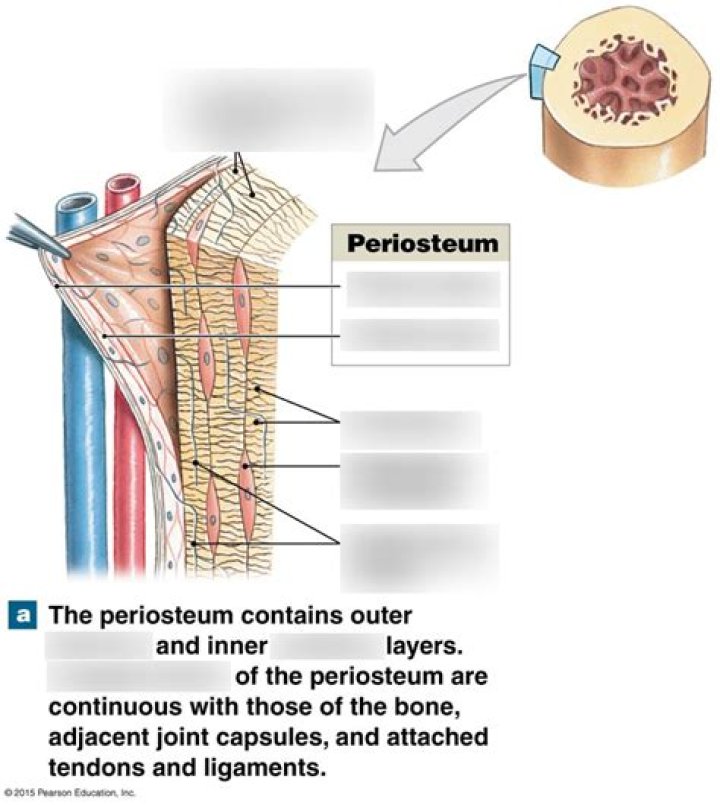
MRI is the preferred imaging modality for identifying MTSS as well as a higher grade bone stress injury such as a tibial stress fracture. Nuclear bone scans are a reasonable alternative but are less specific and sensitive than MRI. MRI findings include periosteal edema and bone marrow edema.
What are 3 causes of medial tibial stress syndrome?
Training errors, shoe wear, and changes in training intensity, duration, and surface can contribute to the development of medial tibial stress syndrome. Risk factors for developing medial tibial stress syndrome include abnormalities of ankle and foot alignment, lower extremity flexibility, and strength.
How do you diagnose a tibial stress fracture?
An MRI is considered the best way to diagnose stress fractures. It can visualize lower grade stress injuries (stress reactions) before an X-ray shows changes. This type of test is also better able to distinguish between stress fractures and soft tissue injuries.
What does a stress reaction in the tibia feel like?
Symptoms are very similar to 'shin splints' with gradual onset pain on the inside of the shin. Individuals suffering from a tibial stress fracture typically feel an aching or burning (localized) pain somewhere along the bone. Swelling may be present at the fracture site.
Which muscle is most commonly associated with medial tibial stress syndrome?
The most common muscles involved in MTSS are the posterior tibialis, flexor digitorum, and soleus muscles. These muscles primarily help stabilize the lower leg and foot and aid in pushing off while running. Another muscle commonly involved is the tibialis anterior muscle.
22 related questions foundHow long does medial tibial stress syndrome last?
It can take anywhere from three weeks to four months. The longer the condition has persisted, the longer it usually takes. Measuring the amount of pain can be important throughout the rehabilitation process.
Can I run with medial tibial stress syndrome?
If it's a stress reaction, the a runner should rest. The trouble is in figuring out which is which or if something else may be going on. Recover Athletics' recommendations for runners with Medial Tibial Stress Syndrome: Temporarily reduce training load (total miles, pace, workouts), to see if things improve.
Do stress fractures show up on MRI?
MRI Scans. An MRI scan can reveal a stress fracture up to two weeks before it's visible on an X-ray. This test uses magnetic fields and radio waves to create two- and three-dimensional images of structures inside the body.
How do you know if you have a stress reaction?
The symptoms of a stress fracture can include:
- Pain, swelling or aching at the site of fracture.
- Tenderness or “pinpoint pain” when touched on the bone.
- Pain that begins after starting an activity and then resolves with rest.
- Pain that's present throughout the activity and does not go away after the activity has ended.
Does a tibial stress fracture require a cast?
A stress fracture of the shin is a thin break caused by repetitive, high-impact exercise. Treatment includes getting adequate rest and backing off intense exercise until it heals. Severe or hard-to-heal fractures may require using crutches, wearing a cast, or surgery. Full recovery can take 4 to 12 weeks.
How can I tell if I have a stress fracture in my foot?
Symptoms of a Foot Stress Fracture
- Tenderness. The injured bone may feel painful or sore when touched; this is called “pinpoint pain”.
- Deep, dull pain. The pain may be felt deep within the foot or toes.
- Weakness. ...
- Intermittent pain. ...
- Swelling. ...
- Changes in biomechanics. ...
- Sharp, localized pain. ...
- Bruising.
Can you walk with a tibia stress fracture?
Doctors do not recommend walking when you have a stress fracture because it may reopen the partially healed fracture, and you may have to begin the recovery process again. Although you can walk, doctors would recommend staying away from hard surfaces and not walking long distances.
How can you tell the difference between shin splints and stress fractures?
How to tell these two conditions apart? With a stress fracture, the pain gets worse as you run and persists in a smaller location after you run, Dr. Goldberg says. With shin splints, pain often occurs over a broad area, although it may be localized, affecting a small area.
How do you fix medial tibial stress syndrome?
Many experts also recommend modifying the training routine, stretching, and strengthening the lower extremity, wearing appropriate footwear, using orthotics and manual therapy to correct biomechanical abnormalities, and gradually return to activity.
Why do shins hurt when walking?
Sore shins are caused by excessively tight and weak anterior tibialis muscles of the front of the shin. If these muscles are tight and weak they will become strained every time you go for a brisk walk.
How can you tell if you have shin splints?
How are shin splints diagnosed? Doctors diagnose shin splints by obtaining a thorough history and by examining you. Your doctor will look at your gait, how you walk, examine your lower leg, ankle and foot. A complete exam will involve moving your ankle and foot around, feeling for tenderness along the bone.
How common are tibial stress fractures?
Risk Factors for Stress Fractures
Tibial fractures are the most common lower extremity stress fracture,1,3 accounting for approximately one half of all stress fractures in children and adults. 1,14 Stress fractures of the tibia are especially common in sports involving running and jumping.
What does a stress reaction look like on an MRI?
MRI. A stress response is characterized by a bone marrow edema like appearance with no obvious fracture cleft or cortical defect and with possible endosteal and/or periosteal edema. A stress reaction might be difficult to differentiate from a stress fracture and in that case, should be called stress injury 1.
Can metatarsalgia cause stress fractures?
Metatarsalgia is more common in the second and third metatarsal bones and the third and forth are more common sites for stress fractures. Several factors play an important role in increasing your risk of developing forefoot pain and metatarsal stress fractures.
Does a stress fracture hurt to touch?
The key symptom of a stress fracture is pain. Depending on the bone affected, it tends to hurt in very specific, pinpoint areas, and it will hurt when you touch the exact area where the bone is broken.
Can a CT scan detect a stress fracture?
Stress fractures often do not show up on X-ray right away. Therefore, other types of diagnostic testing such as magnetic resonance imaging (MRI), computerized tomography (CT) scans, ultrasound, or Technetium-99 bone scans are used to confirm a suspected stress fracture diagnosis.
Do stress fractures hurt all the time?
At first, you might barely notice the pain associated with a stress fracture, but it tends to worsen with time. The tenderness usually starts at a specific spot and decreases during rest.
What are tibia raises?
The tibia raise is an exercise that targets a much forgotten muscle, the tibialis anterior. Strengthening this muscle can be key to solving many different causes of knee pain as well as being proactive in the fight against joint pain.
How long should you rest for shin splints?
Expect that you need at least 2 to 4 weeks of rest from your sport or exercise. Avoid repetitive exercise of your lower leg for 1 to 2 weeks. Keep your activity to just the walking that you do during your regular day.
Does it help to massage shin splints?
If you're suffering from shin splint pain, massage therapy can help with pain relief. The deep tissue strokes release built-up tension, resulting in pain release and the prevention of scar tissue accumulation.