Osteoclasts are formed by the fusion of many cells derived from circulating monocytes in the blood. These in turn are derived from the bone marrow. Osteoclasts may have as many as 200 nuclei, although most have only 5 to 20.
How osteoblasts are formed?
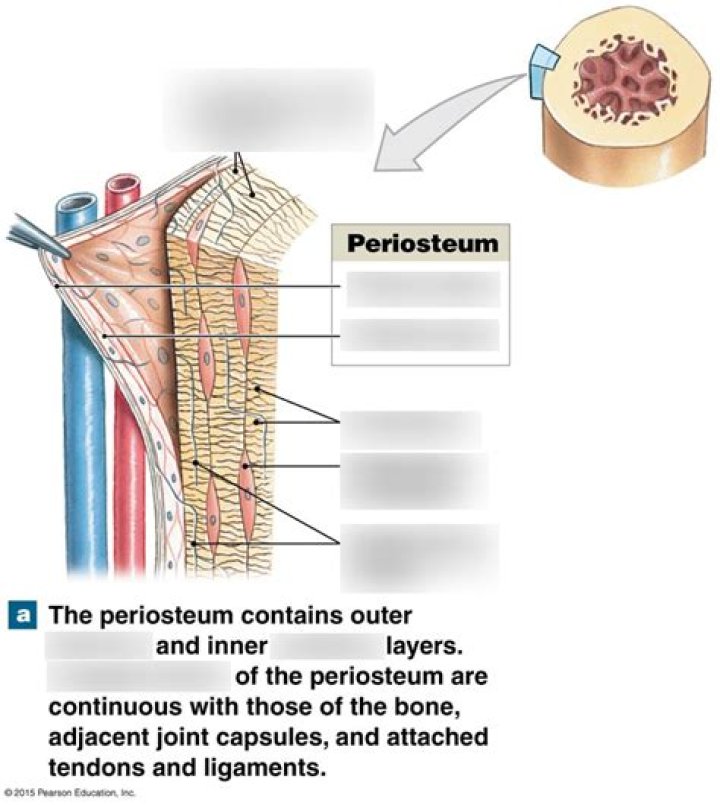
Osteoblasts form a closely packed sheet on the surface of the bone, from which cellular processes extend through the developing bone. They arise from the differentiation of osteogenic cells in the periosteum, the tissue that covers the outer surface of the bone, and in the endosteum of the marrow cavity.
What promotes osteoclast formation?
All aspects of osteoclast formation and functions are regulated by macrophage-colony-stimulating factor (M-CSF) and receptor activator of NF-κB ligand (RANKL), cytokines essential for osteoclast formation and expressed by a variety of cell types, including osteoblast lineage cells.
Where do osteoclasts develop?
Osteoclasts are found on those surfaces of bone which are undergoing resorption. On such surfaces, the osteoclasts are seen to be located in shallow depressions called resorption bays (Howship's lacunae). The resorption bays are created by erosive action of osteoclasts on the underlying bone.
What causes osteoclast?
Without enough vitamin D, your bloodstream will not properly take up the calcium in milk, calcium supplements, or other sources. Low levels of vitamin D will also trigger a series of events that lead to activation of osteoclasts. It also leads to increased production of PTH, which creates even more osteoclasts.
43 related questions foundHow are osteoclast activated?
b, RANKL stimulates osteoclast activation by inducing secretion of protons and lytic enzymes into a sealed resorption vacuole formed between the basal surface of the osteoclast and the bone surface.
What is the function of osteoclast?
Osteoclasts are the cells that degrade bone to initiate normal bone remodeling and mediate bone loss in pathologic conditions by increasing their resorptive activity. They are derived from precursors in the myeloid/ monocyte lineage that circulate in the blood after their formation in the bone marrow.
What are the surface depressions formed by osteoclasts called?
Osteoclasts also participate in the long-term maintenance of blood calcium homeostasis. During bone resorption, the osteoclasts resorb the bone surface forming depressions known as Howship's lacunae.
Do osteoclasts come from osteoblasts?
Osteoclasts are derived from hematopoietic stem cells of the myeloid lineage. Differentiation requires stimulation of the early progenitor cells by the cytokine macrophage colony-stimulating factor (M-CSF) produced by osteoblasts on the surface of bone or by stromal cells in bone marrow.
What is the function of osteoblasts and osteoclasts?
Osteoblast and osteoclast are the two main cells participating in those progresses (Matsuo and Irie, 2008). Osteoclasts are responsible for aged bone resorption and osteoblasts are responsible for new bone formation (Matsuoka et al., 2014). The resorption and formation is in stable at physiological conditions.
Where do osteoclasts reside?
Osteoclasts occupy small depressions on the bone's surface, called Howship lacunae; the lacunae are thought to be caused by erosion of the bone by the osteoclasts' enzymes. Osteoclasts are formed by the fusion of many cells derived from circulating monocytes in the blood. These in turn are derived from the bone marrow.
What is unique about the osteoclast?
The osteoclast, which is the sole bone-resorbing cell, is a unique polykaryon whose activity, in the context of the osteoblast, dictates skeletal mass. All forms of acquired osteoporosis reflect increased osteoclast function relative to that of the osteoblast.
Which hormone increases osteoclast activity to release more calcium ions into the bloodstream?
Two hormones that affect the osteoclasts are parathyroid hormone (PTH) and calcitonin. PTH stimulates osteoclast proliferation and activity. As a result, calcium is released from the bones into the circulation, thus increasing the calcium ion concentration in the blood.
What activates osteoblasts?
Definition and Function of Osteoblasts
In an adult organism, osteoblasts are activated when there is need to regenerate a defect or when the bone matrix has been depleted [6]. Osteoblasts secrete bone matrix proteins, including collagen type 1 alpha 1 (Col1α1), osteocalcin (OC), and alkaline phosphatase (Alp) [6].
What is the role of the osteoblast?
Osteoblasts are specialized mesenchymal cells that synthesize bone matrix and coordinate the mineralization of the skeleton. These cells work in harmony with osteoclasts, which resorb bone, in a continuous cycle that occurs throughout life.
Which cell type becomes an osteoblast?
Key Points. Osteogenic cells are the only bone cells that divide. Osteogenic cells differentiate and develop into osteoblasts which, in turn, are responsible for forming new bones. Osteoblasts synthesize and secrete a collagen matrix and calcium salts.
What are osteoblasts made of?
Bone Cells: Osteoblasts
Osteoblasts are the bone-forming cells that derive from the mesenchymal stem cells of the bone marrow, which also form chondrocytes, myocytes, and adipocytes.
How are osteocytes formed?
Osteocytes form when osteoblasts become buried in the mineral matrix of bone and develop distinct features. Residing within the lacuna of the mineralized bone matrix, osteocytes form dendritic processes that extend out from their cell bodies into spaces known as canaliculi.
How do osteoblasts produce bone matrix?
The osteoblasts secrete the organic matrix, which are dense collagen layers that alternate parallel and orthogonal to the axis of stress loading. Into this matrix is deposited extremely dense hydroxyapatite-based mineral driven by both active and passive transport and pH control.
How does osteoclast attach to bone?
Osteoclasts are giant cells containing between 10 and 20 nuclei. They closely attach to the bone matrix by binding its surface integrins to a bone protein called vitronectin.
How do osteoclast break down bone?
Osteoclasts dissolve bone mineral by massive acid secretion and secrete specialized proteinases that degrade the organic matrix, mainly type I collagen, in this acidic milieu.
Are osteoclasts macrophages?
The Macrophages Are One of the Origins of Osteoclasts. Osteoclasts are well-defined and distinctive in bone marrow, which originate from myeloid progenitor or osteal macrophages and is responsible for bone resorption (18, 19).
What chemical does an osteoblast release that deactivates an osteoclast?
Osteoblasts also secrete collagenase and plasminogen activator [29]. IL-1, TNF, and epidermal growth factor (EGF) have been shown to deactivate osteoblasts and increase release of CSF-1 and RANKL [19, 27].
What means osteoclast?
An osteoclast is a specialized cell that absorbs and removes bone, allowing for the development of new bone and maintenance of bone strength.
What is the difference between osteoclast and osteoblast?
In simple words, an osteoblast builds the bone, whereas an osteoclast eats up the bone so that it can be reshaped into a stronger and resilient load-bearing structure. Other differences are mentioned below. Osteoblasts or lining cells: Osteoblasts are considered the main type of bone cells.